Diabetic Retinopathy
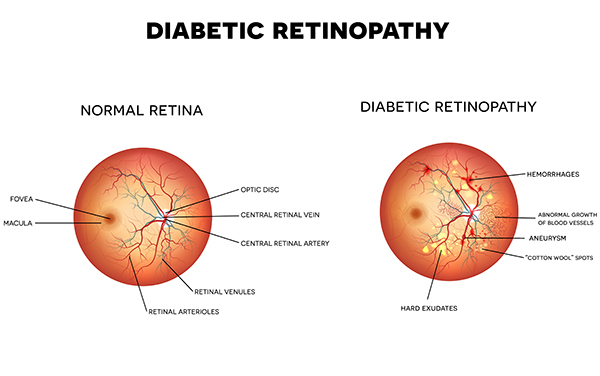 Diabetic retinopathy is the most common diabetic eye disease and is a leading cause of vision loss in American adults. Diabetic retinopathy is caused by changes in the blood vessels of the retina. Small bulges in the blood vessels called microaneurysms are one of the first signs that can be detected. If diabetic retinopathy worsens, a retinal hemorrhage may occur- tiny spots of blood will be visible. When the delicate retinal blood vessels of the macula are damaged, they can leak fluid into the retina causing macular edema. Changes to your vision occur gradually, and may not be noticeable at first. But in its advanced stages, the disease can cause blurred or cloudy vision, floaters, blind spots and eventually blindness. This damage can be irreversible.
Diabetic retinopathy is the most common diabetic eye disease and is a leading cause of vision loss in American adults. Diabetic retinopathy is caused by changes in the blood vessels of the retina. Small bulges in the blood vessels called microaneurysms are one of the first signs that can be detected. If diabetic retinopathy worsens, a retinal hemorrhage may occur- tiny spots of blood will be visible. When the delicate retinal blood vessels of the macula are damaged, they can leak fluid into the retina causing macular edema. Changes to your vision occur gradually, and may not be noticeable at first. But in its advanced stages, the disease can cause blurred or cloudy vision, floaters, blind spots and eventually blindness. This damage can be irreversible.
Diabetic retinopathy is diagnosed by routine dilated eye examinations, which are recommended for any patient with diabetes. Our physicians will carefully examine the retina and will used advanced technology such as retinal photos and OCT scans so that changes of retinopathy will be found as early as possible. If macular edema is present, retinal laser is performed to seal off leaking blood vessels to prevent the condition from worsening. Regular eye exams and laser treatment are proven to slow diabetic retinopathy and prevent vision loss.
The most important factor in preventing vision loss from diabetic retinopathy is prevention of these retinal changes. This is achieved by routine eye examinations and by following the prescribed diet and medications, exercising regularly, controlling blood pressure, and avoiding alcohol and cigarettes.



